Oral Microbiome & Whole Body Health
The oral microbiome is a highly dynamic ecosystem of bacteria, fungi, viruses, and host-derived factors with biological effects that extend beyond the oral cavity. This microbial community is in constant communication with the immune system and plays an active role in regulating inflammatory pathways throughout the body.
When this ecosystem becomes imbalanced—a state known as oral dysbiosis—the effects may extend well beyond the gums. Research increasingly links oral dysbiosis to periodontal disease, cardiovascular disease, metabolic dysfunction, gastrointestinal imbalance, and other chronic inflammatory conditions. These connections reinforce a simple but powerful idea: oral health is not separate from whole body wellness—it is a foundational part of it.
Emphasis is placed on understanding the biological pathways, host microbe interactions, and clinically relevant research that help explain how oral and systemic health are biologically connected. The mouth isn’t separate from the body—it’s one of its most active communication hubs. When the oral microbiome is in balance, it supports health; when it’s disrupted, inflammation can echo far beyond the gums.
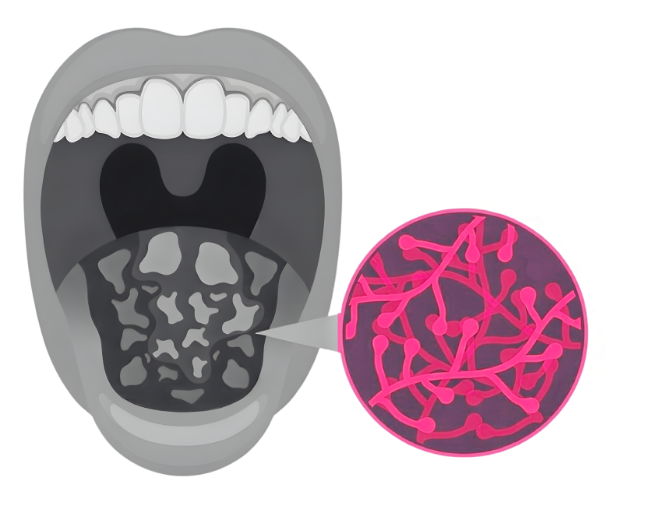
Understanding the Oral Microbiome
Your mouth is home to a living community of microorganisms called the oral microbiome. This ecosystem includes helpful bacteria alongside organisms that can cause problems if balance is lost. When things are working well, these microbes help protect your gums, support healthy tissues, and communicate with your immune system in a way that keeps inflammation in check.
The oral microbiome doesn’t stay confined to your mouth. It interacts closely with the rest of your body through immune signaling, circulation, and digestion. When microbial balance is disrupted—often due to chronic inflammation, stress, diet, dry mouth, or underlying health conditions—the result can be ongoing gum irritation and immune activation that may influence overall health.
In simple terms: what’s happening in your mouth doesn’t stay in your mouth.
How the Oral Microbiome Affects the Whole Body
Immune signaling
Your mouth is one of the immune system’s front doors. A balanced oral microbiome helps train immune cells to respond appropriately. When balance is lost, the immune system may stay in a low grade “on” position, contributing to chronic inflammation.
Metabolic activity
Oral bacteria produce metabolic byproducts that can either support tissue health or promote inflammation, depending on which microbes are dominant. These microbial signals can influence blood vessels, inflammatory markers, and even how the body processes nutrients.
Barrier function
Healthy gums act as a protective barrier. When inflammation weakens this barrier, bacteria and inflammatory molecules can more easily enter the bloodstream. Maintaining microbial balance helps protect this barrier and reduces unnecessary immune stress.
The Big Takeaway
Oral health isn’t just about teeth—it’s about balance. A stable oral microbiome supports healthy gums, calmer immune responses, and better communication between the mouth and the rest of the body. When that balance is disrupted, inflammation can ripple outward in ways that affect overall wellness.
At The Mouth Lab, we like to say:
Don’t just look at the mouth—listen to what it’s telling you.
Saliva as a Diagnostic Tool
Saliva is more than a physiologic fluid involved in digestion—it is a biologically rich medium that reflects microbial activity, immune signaling, and inflammatory status within the oral cavity. Because saliva is in constant contact with oral tissues and biofilms, it provides a dynamic snapshot of what is occurring at the interface between microbes and the host.
In many areas of medicine, noninvasive biomarkers are routinely used to assess risk, monitor disease progression, and guide preventive strategies. Dentistry is now beginning to catch up. Advances in salivary diagnostics allow for the evaluation of specific microbial patterns and inflammatory markers associated with periodontal disease, dental caries, and other oral conditions—often before advanced tissue breakdown or irreversible damage occurs.
Salivary testing can assist in identifying periodontal risk by revealing pathogenic microbial profiles and inflammatory activity that may not yet be clinically visible. In caries management, saliva-based markers related to microbial balance, pH regulation, and protective capacity can help explain why decay risk persists despite good oral hygiene. Salivary diagnostics may also provide insight into conditions such as xerostomia, mucosal inflammation, halitosis, and altered immune response.
Salivary diagnostics provide objective insight into microbial activity, inflammatory burden, and host response—supporting earlier risk identification and more precise management of periodontal, caries, and other oral conditions.
When validated biomarkers are used, salivary diagnostics demonstrate increasing reliability and specificity, allowing clinicians to move beyond symptom based care toward more precise, individualized prevention and management strategies. By integrating salivary data into oral health assessment, dentistry shifts from a reactive model to a proactive, data informed approach—aligning more closely with modern, precision based healthcare.
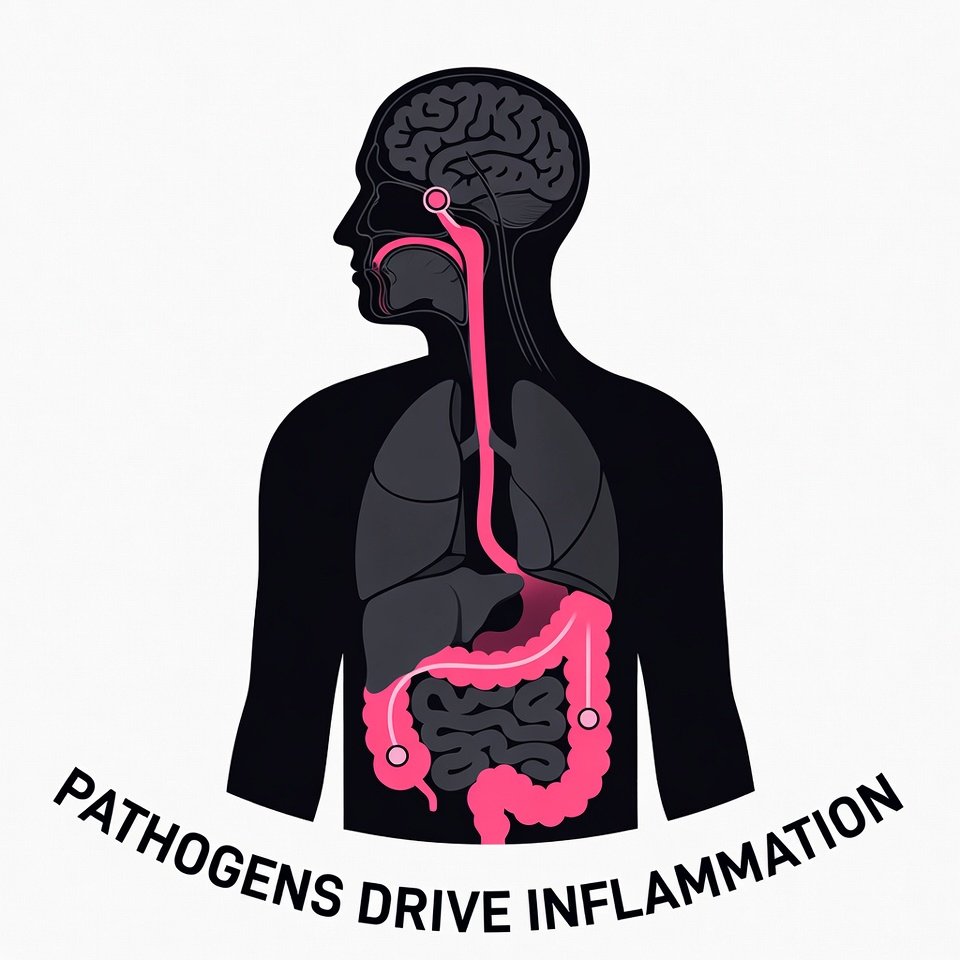
Oral Health and Systemic Connections
Oral inflammation doesn’t stay confined to the gums. When tissues in the mouth are chronically inflamed, such as in periodontal disease, the protective barrier between the oral microbiome and the bloodstream can become weakened. This creates an opportunity for oral bacteria, bacterial fragments, and inflammatory molecules to move beyond the mouth and interact with the rest of the body.
This process, often called microbial translocation, helps explain why ongoing oral inflammation is increasingly linked to systemic inflammation and immune activation. The mouth is highly vascular and immunologically active, making it a key entry point where microbial imbalance can influence whole body health over time.
How Specific Oral Pathogens May Influence Systemic Conditions
Heart and blood vessel health
Periodontal pathogens such as Porphyromonas gingivalis (Pg), Treponema denticola (Td), and Fusobacterium nucleatum (Fn) are strongly associated with advanced periodontal disease. These organisms have been detected in inflamed vascular tissues and atherosclerotic plaques and are known to promote endothelial inflammation and vascular dysfunction.Metabolic health and blood sugar regulation
Chronic periodontal infection involving organisms such as Porphyromonas gingivalis (Pg), Tannerella forsythia (Tf), and Treponema denticola (Td) may increase systemic inflammatory signaling that interferes with insulin sensitivity, helping explain the association between periodontal disease and metabolic dysfunction.Digestive (GI) health
Oral bacteria are swallowed constantly. When oral dysbiosis is present, organisms such as Fusobacterium nucleatum (Fn), Prevotella species, and Treponema denticola (Td) may influence gut microbial balance, intestinal inflammation, and barrier integrity, highlighting the importance of the oral–gut axis.Respiratory health
Oral pathogens including Fusobacterium nucleatum (Fn), Prevotella intermedia (Pi), and Treponema denticola (Td) may be aspirated into the airway, particularly in individuals with periodontal disease, dry mouth, or reduced immune resilience, contributing to respiratory inflammation in susceptible populations.Brain health and cognitive function
Spirochetes such as Treponema denticola (Td), along with Aggregatibacter actinomycetemcomitans (Aa) and Porphyromonas gingivalis (Pg), have been studied for their association with neuroinflammatory processes, vascular changes, and blood-brain barrier disruption. Chronic exposure to these pathogens and their inflammatory byproducts may influence cognitive health over time.Immune and autoimmune conditions
Persistent exposure to periodontal pathogens such as Porphyromonas gingivalis (Pg) and Treponema denticola (Td), both capable of altering immune signaling, may contribute to immune dysregulation and heightened inflammatory responses in susceptible individuals.Pregnancy-related health
Oral pathogens including Fusobacterium nucleatum (Fn), Porphyromonas gingivalis (Pg), and Treponema denticola (Td) have been associated in observational studies with placental inflammation and adverse pregnancy outcomes, underscoring the importance of maintaining oral health during pregnancy.
Translocation of periodontal pathogens offers a biologically plausible mechanism linking oral dysbiosis to systemic inflammation, neuroimmune signaling, and multi-organ disease risk.
It’s important to note that the oral pathogens discussed here represent only a portion of the complex oral microbial ecosystem. The oral microbiome includes hundreds of bacterial species, as well as fungi, viruses, and host-derived factors that interact in dynamic and individualized ways. Likewise, the systemic conditions referenced reflect areas where associations have been most consistently studied, not the full extent of oral–systemic influence.
As research continues to evolve, oral inflammation and microbial imbalance are being explored in relation to a growing range of systemic processes, including immune regulation, vascular health, neuroinflammation, metabolic signaling, and barrier integrity across multiple organ systems. This expanding body of evidence reinforces the concept that oral health should be viewed as a foundational component of whole body health, rather than a standalone concern.
Ongoing Education & Learning Opportunities
The Mouth Lab provides evidence informed education and resources designed to help clinicians, healthcare providers, and individuals better understand the critical connection between oral health and whole body wellness. Emerging research continues to demonstrate that the oral cavity is not an isolated system, but a dynamic biological gateway influencing immune function, inflammation, metabolic health, and chronic disease risk.
Our resources focus on oral microbiome science, salivary diagnostics, and the practical clinical application of oral–systemic research. We explore how microbial balance, host response, and environmental factors within the oral ecosystem can impact periodontal health, cardiovascular health, gut integrity, metabolic regulation, and systemic inflammatory burden.
Through a research driven and education first approach, The Mouth Lab translates complex microbiome and diagnostic science into actionable insights for dental professionals, medical providers, and health conscious individuals. Our goal is to support earlier detection, more personalized care strategies, and a deeper understanding of how oral inflammation and dysbiosis may contribute to whole body health outcomes.
*This page is part of The Mouth Lab’s educational resource library and is intended to serve as a foundational reference on the role of the oral microbiome in systemic health.
